What is Blastocyst and blastocyst transfer ?
A blastocyst is the final stage of the embryo’s development before it hatches out of its shell (zona pellucida) and implants in the uterine wall. Blastocyst transfer is the formulation of new laboratory culture media – the liquid in which the embryo is grown in vitro – has made it possible to “grow” embryos in vitro beyond the typical 2 to 3 day state of development , till they become blastocysts.
The best embryos
Transfer of the embryo on day 5, at the blastocyst stage, has higher pregnancy rates. There may be two possible reasons for this:
- Firstly, transfer of the blastocyst to the uterus may be more physiologically appropriate , since this mimics nature more closely, so that the implantation rate may be higher
- Also, waiting till the blastocyst stage allows the doctor to select the “best ” embryos, since unhealthy embryos are likely to die ( arrest) before they reach this stage.
Less chances of multiple births
Blastocyst transfer also significantly reduces the possibility of potentially dangerous high-order multiple births, such as triplets. Higher implantation rates allows doctors to transfer fewer blastocysts – perhaps only one – reducing or avoiding multiple births and their associated problems. Supernumerary blastocysts can also be successfully cryopreserved using vitrification so that pregnancies can be achieved after thawing.
Why you should insist that your doctor do only blastocyst transfers
In the past, most embryo transfers were done on day two or day three. However, most good clinics have moved on to doing day five (blastocyst ) transfers routinely. Sadly, in India this is still not the standard option , and lots of IVF clinic continue to transfer embryos on day two or three. This is primarily because they’re not very confident about the quality of their laboratory ; and the ability of their embryologist to culture embryos to day five. This is why they prefer putting back the embryos into the uterus, and justify this by telling the patient that the uterus provides a better environment as compared to an incubator. However, this has a lot of disadvantages, and you should insist that your doctor do a blastocyst transfer for you .
For one thing, blastocysts have a better chance of implantation, which means the success rate with blastocyst transfers is higher as compared with Day 2 or 3 transfers. Because they’re more highly developed and have more cells, they have a higher chance of implanting. This also allows the doctor to reduce the number of embryos he transfers, so he can actually transfer just one or two blastocysts, and still have as good a pregnancy rate as compared to transferring three or four Day 3 embryos.
Also, since the doctor is transferring only 1 – 2 blastocysts, you can freeze the extra blastocysts , which means you get a chance to do more cycles . This makes it more cost-effective , because the cumulative pregnancy rate goes up.
Finally, the most important reason you should insist on a Day 5 transfer is because you don’t need to put yourself through that horrible 2 week wait ( 2ww) of not being sure whether you’re going to get pregnant or not if you have poor quality embryos . Thus, if the IVF cycle fails after transferring Day 3 embryos, you never know whether the problem was because the embryo did not develop any further in vivo , or if there was some other reason for the failed implantation. Putting the embryo back too early reduces the pressure for the doctor, because he can claim that at least he did the embryo transfer for you; but you pay the price for this, because you remain in the dark about whether your embryos were able to grow to Day 5. In case the cycle fails, this means you have wasted a chance to get priceless information which could help you to plan your future cycles.
This is specially true for the older woman who has few eggs. This is the group who’s at much higher risk for IVF failure because they are more likely to have embryos which arrest and do not reach the blastocyst stage. Lots of their embryos will have genetic problems, because their eggs are older , which is why they are less likely to implant successfully.
These are the patients for whom a blastocyst transfer is extremely useful. However, they are often poor ovarian responders, and when the doctor collects only 3-4 eggs and therefore gets very few embryos, he is very reluctant to grow them to the blastocyst stage, because he is scared that if the embryos arrest in vitro in the lab, the patient will blame him for the IVF failure. This is why they’d much rather transfer the embryos back in the uterus, and if the cycle fails, they can blame this on ” implantation failure” .
However, after the embryo transfer , the patient is deluded into feeling, “Well, maybe this embryo may implant and become a baby” which is why they are very hopeful during the 2ww.
This false hope is harmful. When the cycle fails, they feel that it was their uterus which rejected the embryo , and then they are advised to go down the surrogacy route. This is bad advice which is completely flawed, because the problem is with the egg and not with the uterus.
Yes, it can be heartbreaking to see your embryos arrest in the laboratory because the doctor tried to grow them to the blastocyst stage. You then have no embryos to transfer at all, and this can be painful. However, the short-term pain is worth it, because of the long-term gain. This gives you a lot of clarity as to what the reason for the failure was, so you can come to terms with it . It’s then much easier to explore find alternative treatment options, rather than muddling around in the dark because you’re completely confused.
Of course, this option requires a very determined patient and a courageous doctor, both of whom understand the risks and benefits of the path they have chosen to explore.
A beautiful Blastocyst on Day 5
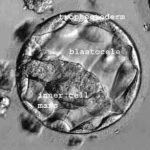
Yoiu can see more images of what good and bad blastocysts look like at http://www.advancedfertility.com/blastocystimages.htm
schematic representation of how Blastocysts are grated at Malpani infertility clinic

What to find an IVF clinic which respects your time and intelligence ?
WhatsApp us at https://wa.me/919867441589/



No comment